Physical therapy guideline for children with malnutrition in low income countries: clinical commentary
Article information
Abstract
Physical therapy intervention along with nutritional rehabilitation has recently become an inevitable combo after recent evidences suggesting a strong interaction between malnutrition and neuro-muscular disabilities which contribute to a significant burden in global settings. Recent studies confirm that appropriate physical assessment of neuro-musculo skeletal system, developmental assessment or cognitive tools along with nutritional assessments followed by exercise rehabilitation will yield positive results in children with malnutrition. There is an obvious need to make available a simple physical therapy exercise guidelines with simple measure and exercise to be used in resource limited settings of developing countries. The purpose of this clinical commentary is to summarize simple assessment tools to evaluate activity impairment, participation restriction, gross motor activity and simple physical therapy intervention program for children with disability secondary to malnutrition.
INTRODUCTION
The prevalence of malnutrition is continuously decreased, however it still remains as a major cause of preventable morbidity and mortality among the young children in many developing countries, especially in African continent. About 50% of all deaths among children aged less than 5 yr can be traced back to under nourishment (Prentice et al., 2016). In most parts of the world malnutrition divulges in the form of undernourishment, which is caused by diet lacking in adequate calories and protein. Child under nourishment is a critical problem in Africa and elsewhere (Harttgen et al., 2013). For instance, poor nutritional status has been a serious problem in Ethiopia for many years and till recent only 4% of children aged between 6–23 months are fed appropriately based on recommended infant and young child feeding. There is also delay in introduction of complementary food to the children (Disha et al., 2012).
For children under 59 months the world wide prevalence are 25%, 8%, and 15% for stunted, wasted and/or underweight respectively. Children in the least developed countries are even more at risk and numbers increase up to 37%, 9%, and 22% for stunting, wasting and underweight respectively (Requejo et al., 2015). Among the overall children in Ethiopia aged between 6–9 months, only half of them receive complementary food. These negative effects are carried into the adult population in this country, where 27% women aged 15–49 yr are thin, with body mass index below 18.5 kg/m2 and 9% are moderately or severely thin. This in turn would lead to more birth of malnourished children. A recent Index Mundi fact sheets indicates that Ethiopia is one of the countries with abundant malnourished children. Moderate-to-severe malnutrition during infancy is associated with a significantly elevated incidence of impaired intelligent quotient (IQ) in adulthood, even when physical growth is completely rehabilitated (Berhan and Berhan, 2014).
But it is worth mentioning that in 2013, Ethiopia achieved the child survival millennium developmental goal by reducing deaths among under-5-yr-olds by two-thirds. So, now it is the appropriate time to focus on curbing physical and neuro-disabilities among malnourished children.
NEED FOR PHYSICAL THERAPY INTERVENTIONS
Incidence of early childhood malnutrition or under nutrition may lead long-term effects like impairment of gross and fine motor skills, easy fatigue, loss of flexibility, impaired rapid sequence movements, behavioural problems, and cognitive impairment like lower attention spans, language impairment, learning disabilities, low IQ scores (Waber et al., 2014). These effects are most likely to be continued into adulthood (Galler et al., 2012). Hence, clinical judgements and rehabilitation program limited to identifying nutritional risk and nutritional supplementations are inadequate in addressing developmental skill of children.
SCOPE AND NEED FOR THIS GUIDELINES
There are ample documentation reporting interplay between neuro-physical disabling conditions and malnutrition. Many studies have reported the effect of malnutrition on growth, cognition, mental and systemic development in children with malnutrition. Literatures even suggest that if malnutrition occurs in the vulnerable period of brain development, it can result in motor impairment (Andrew and Sullivan, 2010; Grantham-McGregor et al., 2007; Kuperminc and Stevenson, 2008). In Africa, however clinical application of assessments of children with physical and neuro-disabilities is seldom practised. In addition evaluating the impact of infantile malnutrition on development in developing countries is inevitably complicated by social context. It is of paramount importance that clinicians in developing countries soon realise that early detection of motor impairments in malnutrition children, followed by early physical rehabilitation will help prevent, minimize and effectively treat physical impairments and motor delay.
A recent audit conducted at Gondar University Hospital, Ethiopia where 362 children were admitted in pediatric ward for severe malnutrition and then referred to physical therapy department for treatment for impairments of which 82.1% were <5 yr old. These children were intervened by developmental stimulation (play therapy), the results showed improvement in self-care domain, mobility domain and aggregate outcomes of the pediatric evaluation of disability inventory (PEDI) score (Gordon et al., 2013). With scarcity of expertise in physical rehabilitation and trained community based rehabilitation (CBR) workers along with resource limiting settings in developing countries, it is vital that the clinicians understand the scope and requirement of clinical physical rehabilitation practice guidelines to screen, refer, and treat malnourished children (Table 1).
Despite the fact there are encouraging clinical outcomes and development of exercise rehabilitation protocols, a tailored exercise rehabilitation guideline for malnourished children in developing countries is notably lacking. At present, physical rehabilitation practice protocols for malnourished children appears to be based on early evidences and conceptions.
DRAFTING OF CLINICAL PRACTICE GUIDELINES
This article reviews the best available evidence-based literature pertaining to assessment and rehabilitation of malnutrition children. In particular the World Health Organization (WHO) homepage, The Ethiopian statistic agency, and a local internal survey audit done at University of Gondar Hospital were also used (De Onis and Weise Prinzo, 2014; Laillou et al., 2014). Using this information in combination with the interdisciplinary expert opinion including present authors, we present a physical rehabilitation protocol for malnutrition children in resource limited setting of developing countries.
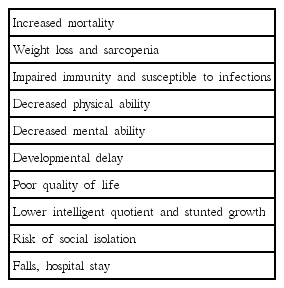
RISK FACTORS, PROGNOSTIC INDICATORS, AND ADVERSE COMPLICATIONS
In low income countries particularly in Ethiopia, children are exposed to multiple risk factors including poverty, maternal depression, poor women education, poor socio economic environment, lower preceding birth intervals, scarcity of health care personnel, low birth weights, underweight mothers, and poor ante natal care (Table 2). Multiple factors which may determine the outcome of a child with malnutrition are; birth weight (normal, 2.5–4 kg), period of breast feeding (normal, ≥6 months), absence of infection, early medical interventions, care giver factors, effectiveness of nutritional programs and quality of life (Campos et al., 2016; Puett and Guerrero, 2015).
Recently, physical activity appears to be an earlier indicator for successful rehabilitation than weight gain. Crookston et al. (2010) observed that children who recovered from stunting in infancy were likely to experience catch-up growth and show no differences in development compared to healthy children (Pulakka et al., 2015).
ASSESSMENT OF CHILDREN WITH MALNUTRITION
A well integrated holistic assessment which includes medico-nutritional plans of management or advice along with physical therapy intervention plans is most likely to improve outcomes (Gladstone et al., 2014; Trehan and Manary, 2015). Very little is known about parenting practices in Ethiopia, most studies report low level of education and unawareness among mother in many African countries. Many researchers reported maternal-child interaction as an important factor in childhood malnutrition and also recommend Socio Emotional Development Scale as a suitable assessment tool for African settings (Cooper et al., 2009; Stewart et al., 2011).
Subjective assessments are important domain in guiding the physical examination and anthropometric measurements. Tools like subjective global assessment (SGA), mini nutritional assessment, and subjective global nutritional assessment (SGNA) score for children can be used (Secker and Jeejeebhoy, 2012; Steenson et al., 2013). The SGNA is a simple pediatric nutritional risk score; consisted of nutrition oriented physical examination and information on the child’s recent and current height and weight, parental heights. The SGA tool consisted of features identifying nutritional risks, gastrointestinal symptoms, functional capacity, and physical examination like loss of subcutaneous fat, muscle wasting, ankle edema, sacral edema, and ascites. From a clinical point of view, these tools allow a quick and valid assessment suitable for practice.
With recent evidences reporting association between neuro developmental delay, neuro disabilities and malnutrition (Gladstone et al., 2014). Programs to improve malnutrition will be most effective if they also target the neurodevelopment of children. Depending on the type of malnutrition brain is affected in different ways; for example chronic malnutrition (stunting is manifested as low height for age), acute malnutrition (formerly known as protein-energy malnutrition and manifested as either kwashiorkor or wasting, low middle-upper arm circumference [MUAC] or low weight for height), or a specific micronutrient deficiency such as iron or zinc. Some deficiencies, such as chronic malnutrition, will affect global functioning of the brain and are assessed best through general developmental assessment tools (Aly and Taj, 2010; de Moura et al., 2010).
The quality of stimulation at home can be better measured by the modified version of the Infant/Toddler HOME (Home Observation for Measurement of the Environment) inventory developed by Bangladeshi scholars suitable for many low resource settings. The modified version of inventory contains 60 items and six subscales: (a) organisation of the physical and temporal environment, (b) stimulation (opportunities for variations in daily stimulation at home), (c) maternal involvement with the child, (d) play materials, (e) avoidance of restriction and punishment, and (f) Emotional and verbal responsivity of the mother. The total score was calculated by summing up all positive responses (Nahar et al., 2012).
Other deficiencies such as iron deficiency may have more effect on neural myelination and tools to assess processing speeds may be more useful. A neurologic examination should include assessment of tone, cranial nerve problems (particularly swallowing difficulties), head circumference, and dysmorphic features to help in understanding any underlying etiology for the child’s condition.
ASSESSMENT OF PARTICIPATION AND ACTIVITY LEVEL
PEDI is a comprehensive validated tool in the assessment of key functional capabilities and performance of children aged 6–90 months (0.5–7.5 yr). It assesses the functional ability in three domains; self-care, mobility and social functioning of the child. PEDI is an easy and quick way assessment tool of children abilities with scoring of 0 or 1. Moreover, PEDI is more adaptable and easily translatable to the context of cultures (Dumas et al., 2015).
A child with malnutrition can show delayed gross motor function as one of the associated problems. Motor development can be assessed using various tools like the Bayleys scale, the Denver II scale, the Peabody scale, Alberta Infant Motor Scale (AIMS), the Movement Assessment of Infants, the Test of Infant Motor Performance, Gross Motor Function Measure, Differential Ability Scales-II, etc., AIMS, based on neuro maturation concept and dynamic theory, is a quick observational assessment tool used to evaluate the motor development in infants between the ages of 0 to 18 months. It is comprises of 58 items observed in four different positions (i.e., prone, supine, sitting, and standing). It is a reliable (r=0.85 to 0.97) and valid (sensitivity, 80%; specificity, 90%; positive predictive value, 70%; and negative predictive value, 80%) tool. AIMS is a useful tool in assessing the six child growth standards set by the WHO. These include sitting without support, hands-and-knees crawling, standing with assistance, walking with assistance, standing alone, walking alone. According to the scores of AIMS, a percentile rank below 10 is considered to be atypical performance, between 11–25 is considered as suspected performance, between 26–75 is normal, 76–90 is very good performance and between 90–100 is excellent performance (Iyer et al., 2003; Maia et al., 2011).
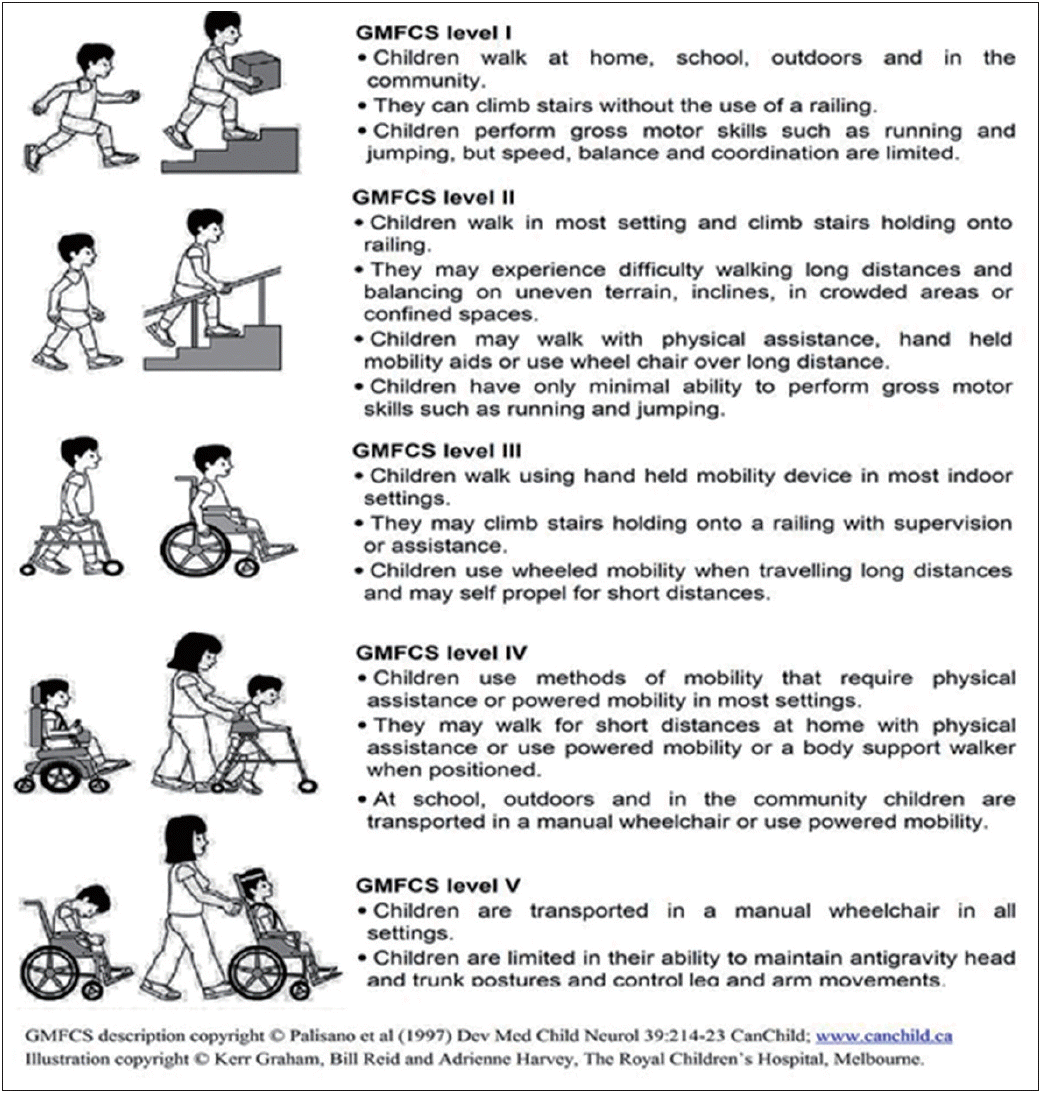
It is important to remember that the severity of children motor disability is usually associated with feeding difficulties. Physical therapy evaluations shall include ability to sit, ability to use of assistive devices and positioning in severe children. Gross Motor Functioning Classification System (Fig. 1) which is a broad 5-category system for defining motor functional limitations and abilities can be an easy useful adjunct tool in this context (Gladstone et al., 2014; Hiratuka et al., 2010).
ASSESSMENT BASED ON BODY FUNCTIONS AND STRUCTURE LEVEL
Through observation will be one of the key components in the assessment of malnourished children. Among the two specific kinds of malnutrition that is marasmus (severe wasting) and kwashiorkor (Oedematous). In marasmus signs such as prominent bones (rib rosaries), skinny limbs, loose skin especially in the buttock region (buggy pants) can be noticed. In kwashiorkor bilateral pedal edema, hair color changes, dermatosis and protuberant belly are seen. Other signs to look for during the general examinations are depigmentation, hyperpigmentation of skin, general pallor, kolionychia in iron deficiency. Measuring the MUAC using tape is a quick and simple way to determine whether or not a child is malnourished using a standard colored plastic strip. MUAC is suitable to use in children from the age of 12 months up to the age of 59 months. However, it can also be used for children as young as 6 months with length above 65 cm. Even head circumference measure may imply an under lying neuro diagnosis (Goossens et al., 2012).
The locomotor system examination will surely help gauze the motor disability of the child. Children should be assessed for muscle wastings, decreased muscle strength, child’s tone which can sometimes be stiff or floppy differentiation of which would aid in positioning splinting eventually good feeding. In presence of bipedal pitting edema grade them; grade 1 edema (only feet), grade 2 (up to knee), and grade 3 (above knee). Mobility of the joint should be examined for hypo and hypermobilities using range of motion measuring tools like goniometer (Laillou et al., 2014).
PHYSICAL THERAPY INTERVENTIONS FOR MALNUTRITION CHILDREN
The routine care or medical managements for malnutrition is well established and discussed enough in many studies. A cheerful environment which is stimulating, structured play therapy, progressively increasing physical activity, and mother’s involvement in care of the child are important components of therapy. Low cost and culturally appropriate homemade toys, lent toys, picture books, parental education to make mothers more effective in teaching their children and enhancing maternal child interactions; mothers responsiveness to their infants and playing, chatting, singing, showing love and incorporating playing in daily activities such as bathing, dressing and feeding to improve development. It is important to advice mothers to avoid physical punishments.
Physical therapy intervention in malnutrition children holds paramount importance, if we are to reduce neuro-musculoskeletal and developmental disabilities. Physical interventions ideally should begin after the child medical conditions are stable. The aims of physical activity or play therapy are mentioned in Table 3. The WHO structured play therapy sessions will address these aims to physically treat malnutrition children (Appendix 1).
In practice and implementations of early stimulation program (Appendix 2) the family will hold the highest ‘responsibilities, so as the child will have more time of stimulation and achieve the aim of the treatment. The role of CBR in parental education and helping the parents to insure the continuity of the stimulation therapy will be crucial in low income countries. Some of the areas of stimulation include; movement, body control, strength, balance, use of the hands, the senses, communication, interaction with other people, basic activities for daily living, observing, thinking, and doing.
CONCLUSIONS
Physical activity and exercise prescription in line with neuro motor disabilities and health profile of the malnutrition children is seldom practiced in resource limited settings. Instead, it is advised to initiate early exercises and physical therapy interventions in malnutrition children with tools made of simple available materials to encourage stimulation and play. In addition community based parental education and play activities with food supplementations should be initiated.
Notes
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.