Factors associated with physical activity of women aged over 75 in South Korea
Article information
Abstract
Physical activity (PA) and the activity-related factors of aged women dwelling in a city community of Korea were examined for 253 participants aged over 75, regarding their socio-demographic characteristics, health status, physical performance, depression, cognitive function, self-efficacy, outcome expectations, and PA. Descriptive statistics, analysis of covariance, Pearson correlation, and multiple regressions were performed to analyze cross-sectional data. The data indicated the participants carry out low-intensity physical activities, such as house chores, light gardening, and walking for pleasure. Moderate and vigorous-intensity physical activities were performed rare. The frequency per week was 15.62±8.60 for all listed activities. Frequency of PA decreased significantly in participants aged over 80, of poor perceived health, depression, and cognitive decline. There was a negative correlation between PA and the figure 8 walks (r=−0.20, P=0.002). PA showed significantly positive correlation with self-efficacy (r=0.34, P=0.001) and outcome expectations (r=0.36, P=0.001). In a regression analysis, explanation rate of factors influencing PA was 21.9 % (P=0.001). Outcome expectations (β=0.23), cognitive function (β= −0.20), and self-efficacy (β=0.19) influenced the PA. These findings indicate that interventions stimulating cognitive function and enhancing positive expectation and self-confidence should be included for PA promotion of older women aged 75 years and over.
INTRODUCTION
As the life expectancy of older adults continues to increase they comprise the fastest growing segment of the population in high-income countries, South Korean women, for an example, are projected to be over 86.7 years in 2030 (Kontis et al., 2017). The rapid rise of older population is projected to increase proportion of chronic disease and life dependency (McPhee et al., 2016). It poses an important public health challenge to maintain the quality of life and to functional independency in their later life due to the extended life span (Katz et al., 1983).
Physical activity (PA) of older adults is a key for the improvement of cardiovascular, musculoskeletal and psycho-social health, cognitive and physical functioning (Taylor et al., 2004). Despite these benefits, PA of the elderly women is generally of a low intensity and tend to confine housework and less vigorous activities than men (Giuli et al., 2012), and it is more obvious with advancing age (Keadle et al., 2016). This suggests that women aged over 75 may be a focused target population when considering PA intervention studies for healthy aging.
Several studies have investigated the socio-demographical, physical and psychological correlates of PA of older women. It was shown that age, income, and education level significantly correlated with PA (Lin et al., 2017), so were the subjective health status (Eifert et al., 2014) and lower-extremity function (Aoyagi et al., 2009). These studies, however, provided insufficient evidences to examine whether these factors predict the PA of women over 75 years. The relationship between depression and PA may be bidirectional (Ku et al., 2012). In a systematic overview of meta-analysis, exercise significantly reduces depressive symptoms (Catalan-Matamoros et al., 2016). Only two studies showed that depression predicts PA in older adults over 65 years (Giuli et al., 2012; McKee et al., 2015). It is also necessary to investigate whether depression is a significant predictor for women over 75 years. When compared with the PA group of elderly females, cognitive function of the highest PA group was significantly less decreased (Yaffe et al., 2001). A previous study demonstrated that cognitive function was a good predictive of PA (McKee et al., 2015), although other studies have found that cognitive function did not affect PA (Ferreira et al., 2010; Giuli et al., 2012). Another study (Zhu et al., 2017) reported that moderate-intensity PA reduces the risk of cognitive impairment. There seems a bidirectional association between PA and cognitive function but more information is needed whether the cognitive function predicts PA. Elderly women aged 75 and older mostly demonstrate a low intensity PA rather than a moderate intensity PA; thus, further studies are needed to understand the relevance of low-intensity daily PA to cognitive function (Beckett et al., 2015). Self-efficacy has been considered related to PA (Bauman et al., 2012) and outcome expectations are also reported to affect exercise participation and PA in older adults (Resnick, 2001). It was reported that the strongest predictor of health behaviors in elderly women is self-efficacy, followed by outcome expectations (Conn, 1997). Studies of the physical activities of middle-aged and elderly women in Taiwan revealed that self-efficacy has a significant correlation with PA, but not in a regression analysis (Lin et al., 2017). In another study, PA increases significantly when having high self-efficacy, not outcome expectations (Mielenz et al., 2013). These findings indicate a need for further study for the influence of self-efficacy and outcome expectations on PA of older women.
Specifically, only few studies have included a multivariate evaluation of factors related to PA focused on older women in their later stage. Thus, there is a need to investigate the effects of subjective health status, physical performance, depression, cognitive function, self-efficacy, and expectation on the PA of older women in their later life stage in particular.
In this context, aims of this study were to investigate the PA frequency of a sample of community-dwelling older women over 75 in South Korea, and analyze the predictors of PA. Results identifying the current state and predictors of PA can provide basic data for the design of intervention programs to enhance PA in this population.
MATERIALS AND METHODS
Study setting and participants
Study participants were recruited from elderly women registered at one senior club and three senior centers in the Daegu city of South Korea. Study inclusion criteria were as follows: (a) women aged over 75, (b) who replied independently on the questions about their activities of daily living (eating, bathing, getting dressed, using the bathroom, moving, walking), (c) who were capable of communication and social activity, (d) who volunteered to participate in this study, and (e) who did not participate in any other structured PA program.
A sample size greater than 252 people was needed for an one-way analysis of variance using a test power of 0.95, a significance level of 0.05, and a medium effect size (Faul et al., 2009). Initially, 278 older women were included from the accessible population (1,470 total individuals). However, 25 individuals provided insufficient responses or did not complete the questionnaires. Therefore, the final analysis was conducted for data collected from 253 participants.
This study was approved by the Institutional Review Board of Kyungpook National University (approval number: KNU 2016-28).
Measurements
The participants were assessed for the general characteristics including age (75–79, 80–84, or 85 years and over), level of education (illiteracy, elementary school or higher), living arrangement (alone, or not alone), perceived economic level (low, middle, or high), comorbidity (yes, or no), and subjective health status (very good, good, moderate, poor, or very poor).
The figure-8 walk test (F8WT) is a measure of walking skills in daily life (Hess et al., 2010). Individuals were asked to walk a figure 8 around two cones placed 1.5 m apart. The participant was instructed to stand at the middle point between the two cones and to begin walking at a usual pace. The pattern consisted of walking on curved paths, clockwise and counterclockwise, with straight-path walking between the curved paths. One trained investigator recorded the time to complete the F8WT. A longer time to complete the task is considered poorer performance.
Depressive symptoms were measured using the Short Geriatric Depression Scale developed by Yesavage and Sheikh (1986). Total scores were obtained by adding one point for each response that was symptomatic of depression, resulting in a score ranging from 0 to 15, with higher scores indicating greater depressive symptoms. A score ≥5 (cutoff value) suggests depression. Cronbach α was 0.91 for this study.
The Mini Mental State Examination measured cognitive function (Folstein et al., 1975). It is composed of items such as orientation, registration, attention and calculation, recall and language. We used the total score, which ranged from 0 to 30 points, with higher scores indicating better cognitive function. The score below 24 indicates cognitive impairment. Cronbach α for this study was 0.94.
Self-Efficacy for Exercise developed by Resnick and Jenkins (2000) is a 9-item questionnaire regarding the ability to continue exercising despite barriers, with scores ranging from 0 (not confident) to 10 (very confident). Items include asking participants how confident they are in exercising when they are having pain or; fatigue or in busy or stressful situations. It is scored by summing the numerical ratings for each response and dividing that value by the number of responses. A higher score represents better self-efficacy. Cronbach α for this study was 0.84.
The Outcome expectations for exercise 2, which anticipates the consequences of a given behavior, developed from the study of Resnick (2005) focuses on the perceived consequences of exercise for older adults. The questionnaire consists of 13 items measuring nine positive and four negative outcomes expectations. The test uses a 5-point scale, ranging from 1 (not at all) to 5 (absolutely agree). It is scored by summing the numerical ratings for each response and dividing this value by the number of responses. A higher score indicates positive expectations for the outcomes. Cronbach α for this study was 0.89.
PA was assessed using the questionnaire for the Community Health Activities Model Program for Seniors developed by Stewart et al. (2001). This measurement assesses the frequency of different activities and ranges from light to vigorously intense activities, which was completed in a typical week over the past 4 weeks. Participants reported whether they had engaged in each activity (yes/no), and the frequency per week.
Data collection
The data collection for this study consisted of one-on-one interviews and measurement by trained research assistants from March 11 to April 28, 2016. A verbal presentation was given by the investigator to the board regarding the research purpose and overall study procedure. All participants voluntarily agreed to participate in the study and signed an informed consent after receiving information about the study goal, data collection, and confidentiality. Participants were told that the data collection process could be terminated at any time without penalty. Investigators were trained on the survey methods and direct measurement methods to ensure consistent measurements prior to the investigation.
Data analysis
The collected data were analyzed using IBM SPSS Statistics ver. 21.0 (IBM Co., Armonk, NY, USA). Descriptive statistics were used for general characteristics, study variables such as physical performance, depressive symptoms, cognitive function, self-efficacy, outcome expectations, and PA. The analysis of covariance (covariance; age) was used to examine the difference in PA according to general characteristics. Pearson correlation coefficient was used to determine the relationships between measured variables. Multiple regression analyses were performed to determine the predictors of PA among older women. The categorical variable was changed to a dummy variable before the analysis.
RESULTS
General characteristics of the participants
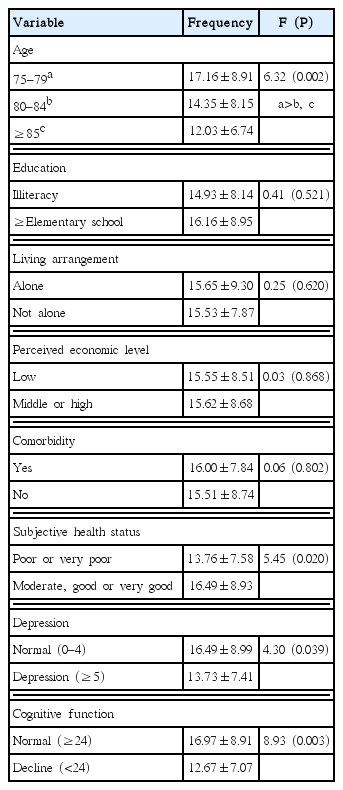
The average age of the 253 participants was 79.8 years (age range, 75–94 years). In addition, 53.7% of the subjects had education higher than the elementary school, 49.8% were living alone, and 58.5% were economically above the average. Furthermore, 83.8% of the participants had chronic diseases, such as hypertension, diabetes, and arthritis. In all, 67.2% of the participants had a moderate or better subjective health status. For the F8WT, 57.3% of the subjects belonged to the average or higher groups, and the mean score of the F8WT was 42.7 sec. Regarding the presence or absence of depressive symptoms, 67.6% of the patients had no depressive symptoms. The mean score of depressive symptoms was 3.4/15. Furthermore, 68.0% of the participants belonged to the normal group in terms of cognitive function. The mean score for the MMSE was 24.9/30. The mean scores of self-efficacy and outcome expectations were 46.2/90 and 51.7/65, respectively (Table 1).
PA of the participants
The frequency of PA in participants was 15.6 times per week. Light work in the house (sweeping) was as frequent as 4.6 times per week, followed by walking leisurely for pleasure 3.6 times per week. PA related to recreation/leisure activity and aerobic/exercise activity was found to be very rare with the exception of walking (Table 2).
PA according to the general characteristics of the participants
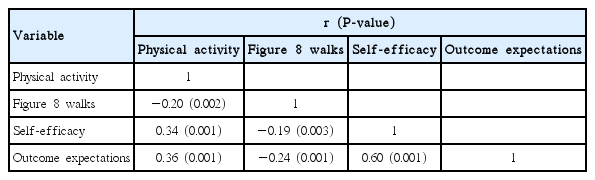
The mean score for PA differed significantly depending on the age (F=6.32, P=0.002). The 75- to 79-year-old age group showed higher scores of PA compared with the other age groups. When the results of the analysis of PA by general characteristics were adjusted for age (covariate), individuals with a moderate or better level of subjective health status showed a higher frequency of PA compared to the other groups (F=5.45, P=0.020). Compared to the depressed group, the nondepressed group showed a significantly higher PA (F=4.30, P=0.039). The group with normal cognitive function had significantly higher PA compared to the cognitive dysfunction group (F=8.93, P=0.003) (Table 3). There was a negative correlation between PA and F8WT (r=−0.20, P=0.002). A positive relationship was found between self-efficacy and PA (r=0.34, P<0.001), and between outcome expectations and PA (r=0.36, P<0.001) (Table 4).
Predictors of PA
To identify the factors that affect the PA of elderly women, multiple regression analysis was performed using age, subjective health status, F8WT, depression, cognitive function, self-efficacy and outcome expectations. The model was significant, explaining 21.9% of the variance in PA (F=9.80, P=0.001). Among these, outcome expectations (β=0.23, P=0.002) was the strongest predictor, followed by cognitive function (β=−0.20, P=0.002), and self-efficacy (β=0.19, P=0.007) (Table 5).
DISCUSSION
The aim of this study was to identify PA and it’s predictors among community-dwelling older women aged over 75 years. The frequency of all PA was 15.6 time per week. This finding is slightly higher than the 13.3 times per week for the American women as reported in the study by Stewart et al. (2001). The participants in this study were found to perform mostly low-intensity activity (2–2.5 metabolic equivalent of tasks [METs]), such as household chores and light walking, whereas moderate-intensity activity (3 METs) was not performed or performed less than once per week. The participants do not engage in PA appropriate for maintaining and promoting health. World Health Organization (2010) recommended at least 150 min per week of moderate-intensity PA for health benefits in older adults. It is consistent with the data obtained in previous studies, in which older women performed daily domestic activities such as walking and housework (Plonczynski et al., 2008). It suggests the possibility of developing functional dependence among women over 75 years old in the future and of becoming vulnerable elderly, which reduces the quality of life related to health. Therefore, it is important to develop a strategy that could involve women over 75 in moderate intensity PA.
Women of 85 years and over performed lower PA than those of 75–84 years in this study, which is consistent with another study (Eifert et al., 2014). But age was not a significant predictor of PA in the the regression model. Participants with good subjective health status had significantly higher PA than those with poor subjective health status, which was consistent with previous studies (Browning et al., 2009; Eifert et al., 2014; Giuli et al., 2012). Nevertheless, subjective health status was not a significant predictor of PA among older women in the regression model. This result was different from another study that subjective health status predicted PA in Italian elderly (Giuli et al., 2012). Because of insufficient information on PA of older and oldest old women, there is a need to study further for determining whether subjective health status leads to perform more PA in older women. Although non-depressed participants performed PA more than the depressed, depressive symptoms were not a significant predictor of PA in the current study. The results were inconsistent with previous studies (Giuli et al., 2012; McKee et al., 2015) that depressive symptoms predicted PA significantly. Depressive symptoms affect the level of physical functioning and physical functioning leads to more PA (Giuli et al., 2012). On this basis, it is considered that depressive symptoms do not affect PA directly because most participants in this study showed no problems of physical functioning.
In this study, PA was lower in the cognitive decline group than in the normal group and cognitive function was a significant predictor of PA. Cognitive function is an important factor to perform more PA because it is associated with independent daily activities such as judgment and executive function (de Guzman et al., 2015). The finding is consistent with the notion that preexisting cognitive impairment cause a reduction PA (Weuve et al., 2004) and cognitive function of older adults affects PA significantly (de Guzman et al., 2015; McKee et al., 2015). It shows that intervention for maintain and promoting cognitive function could activate PA.
Walking is a complex exercise technique based on a variety of balance-control abilities, and a brain-body interaction allows walking and rapid adaptation to change depending on the circumstances (Capaday, 2002). The F8WT is a valid tool to assess walking performance and balance in older adults (Hess et al., 2010). In this study, there was a negative weak correlation between the F8WT and PA, but F8WT was not a significant predictive factor of PA. Self-efficacy is a person’s confidence in one’s ability to perform a certain behavior successfully (McAuley et al., 2011). A significant positive relationship was found between PA and self-efficacy and self-efficacy predicted PA in this study. People who have higher self-efficacy tend to hold more positive attitude toward exercise and to engage in more PA (Ayotte et al., 2010). This finding was similar to the results obtained by Morris et al. (2008), which also showed a positive correlation between self-efficacy and PA. Therefore, it is necessary to apply a program emphasizing self-efficacy to promote PA. Outcome expectations are the beliefs that performing a specific behavior will lead to a desired outcome. Stronger positive outcome expectations were associated with a greater frequency of PA in the current study. This result is consistent with those obtained from PA studies of older adults (Resnick, 2001; Williams et al., 2005). This finding suggests that participants-more confident in overcoming obstacles and more knowledgeable about the benefits of PA,-perform PA more frequently. Consequently, positive outcome expectations can be considered a target of intervention which would increase PA in older women.
Several limitations should be considered when interpreting the findings of this study. First, the study participants were community-dwelling older adults who were mostly independent in daily living. Therefore, the results cannot be generalized to more disabled women. Second, PA assessment was based on a self-reported questionnaire, which may be subject to a recall bias; although, using subjective measurements among older adults can be valid (Colbert et al., 2011). Despite of these limitations, this study provides cognitive function, self-efficacy and outcome expectations as useful factors in the development of effective interventions to increase PA in older women. Therefore, there is a need for a systematic PA program that can increase the current low-intensity activity to moderate-intensity activity to provide health effects in elderly women. As a strategy to promote PA, a PA program needs to include education about the positive incentives for facilitating PA and strengthen cognitive stimulation and self-confidence motivating PA.
Notes
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.
ACKNOWLEDGMENTS
This research was supported by grant from the National Research Foundation of Korea (NRF) funded by the Korean government (NRF-2015R1C1A2A01052834).